“You can and you will!”
This quote was written on the wall of Sean Noble’s room in intensive care, where he spent two months on life support after being infected with COVID-19 in September 2021.
Noble, then 44, caught the virus from his daughters. Although they recovered, his sickness progressed rapidly. He had low energy and a sore throat for about a week, but most concerning was that he was finding it harder to breathe as the days passed. He and his wife monitored his oxygen saturation, and when it fell below 90 percent, they headed to the emergency department.
A former college soccer athlete, Noble’s immune system went into overdrive after he contracted the virus and kept attacking his lungs even after the virus was gone.
“It’s not always the virus itself that does the damage, but the patient’s immune system’s response to the virus. The patient just gets super, super sick, and then the immune system just goes haywire trying to combat the virus. That’s what ends up causing a lot of the lung damage,” says UNC Health transplant nurse practitioner Christina “Tina” White, MSN.
Noble ended up with fibrosis of the lungs (pulmonary fibrosis), which occurs when lung tissue becomes damaged. The lung damage caused by pulmonary fibrosis can’t be repaired.
“My lungs were permanently scarred,” Noble says.
ECMO: Bypassing the Lungs
By the time Noble was admitted to the ICU, doctors needed to take drastic measures to save his life.
“Sean came into us pretty sick and was having a hard time breathing, so in addition to a traditional ventilator, he also needed ECMO,” says UNC Health lung transplant surgeon Benjamin E. Haithcock, MD, surgical director for lung transplant at UNC Hospitals.
ECMO, or extracorporeal membrane oxygenation, temporarily takes over the work of the heart and/or lungs so those organs can rest and heal. The patient’s blood is pumped into a heart-lung machine that removes carbon dioxide and sends oxygen-filled blood back to tissues in the body.
Noble was on ECMO for six weeks to give his lungs a chance to recover on their own.
Awake and Walking on ECMO
 After about 30 days, Noble’s care team determined he would need a double lung transplant to survive. Then they had to make sure he was in good enough physical shape to get the transplant.
After about 30 days, Noble’s care team determined he would need a double lung transplant to survive. Then they had to make sure he was in good enough physical shape to get the transplant.
“We want patients up and ambulating (walking) when they’re on ECMO to make sure that they maintain adequate muscle strength to tolerate the surgery,” White says. “We also assess their heart, kidneys and other organs to be sure that everything looks OK and that they can tolerate the procedure.”
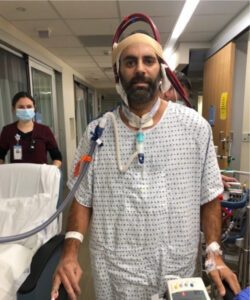
So, three times a day for two weeks, Noble walked the unit while still hooked to ECMO.
“I had a tube from my heart wrapped around my head, and it took five people to walk me for 15 minutes, and probably took them 15, 20 minutes to hook everything up, get everything ready, and then get me back into bed,” Noble says.
A Double Lung Transplant for Thanksgiving
 Once his care team determined that a double lung transplant was his only chance of survival and that his body was strong enough to tolerate the procedure, Noble was placed on the lung transplant list.
Once his care team determined that a double lung transplant was his only chance of survival and that his body was strong enough to tolerate the procedure, Noble was placed on the lung transplant list.
And on Nov. 15, two weeks after being placed on the list, Noble received a double lung transplant.
“We got him off ECMO immediately after his transplant in the operating room—the lungs work as soon as we implant,” Dr. Haithcock says. “Seeing the folks who undergo a lung transplant be able to breathe so easily after their operation is an amazing gift.”
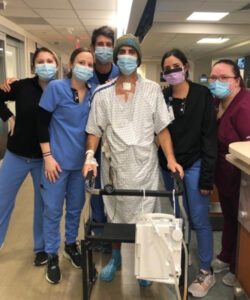
Noble came off the ventilator soon after. And 10 days later, the day after Thanksgiving, Noble went home.
Life with New Lungs
 Nearly 18 months after his transplant, Noble says he is 90 percent back to where he was before—enjoying raising two girls, ages 7 and 10, with his wife of 13 years, Lisa.
Nearly 18 months after his transplant, Noble says he is 90 percent back to where he was before—enjoying raising two girls, ages 7 and 10, with his wife of 13 years, Lisa.
He recently coached his youngest daughter’s soccer team in the Futsal League, he exercises daily, is back to lifting weights and works from home as a project manager for Lenovo’s North American sales team.
“Life is good,” he says.
Still, he and his family have to be careful to minimize his risk of any infection, especially from COVID-19, so they try to spend time with others mostly outdoors.
“While the newer variants don’t seem as fatal, they are very transmissible, and given what happened last time, I have to be very cautious because I am immunocompromised,” Noble says. “Still, receiving a lung transplant saved my life and will allow me to spend many more quality years with my wife and two young daughters. I am forever grateful to my donor, their family, and the outstanding transplant team at UNC Hospitals.”
Learn about transplant care for adults and children at UNC Hospitals. Register to be an organ donor today.

