Sherry Flynn, 47, is an outgoing mother of two who enjoys spending time with her family and friends, traveling to watch her son play baseball and attending church.
“I like family time and having lots of friends over for cookouts,” Flynn says. “Church is a big part of my life, and I enjoy playing and watching sports.”
All of that came to an abrupt stop 10 months ago when Flynn contracted COVID-19 in early December 2020.
“I started having flu-like symptoms, and then about four days later I woke up and I felt like I couldn’t breathe or move,” Flynn says. “I felt a heavy, almost paralyzed feeling.”
Flynn’s fiancé called for an ambulance.
A Lonely Ward
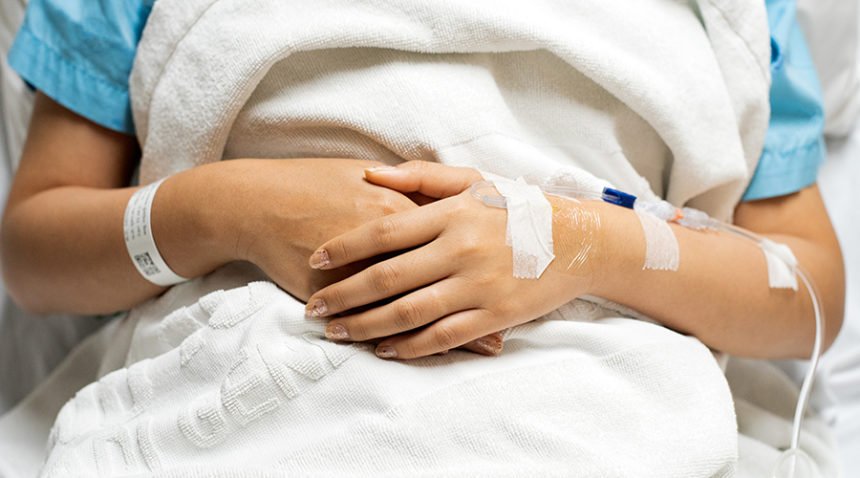
Flynn was hospitalized at Wayne UNC Health Care for 13 days, taking several types of medication and receiving supplemental oxygen.
The first week she was hospitalized, Flynn felt too sick to do anything, even use her phone or watch TV.
“I didn’t even want to lift my head,” Flynn says. “And being in that hospital was so lonely because nobody can be around you. You’re cut off from everything, and your brain doesn’t function like it should because of the lack of oxygen—it has a real effect on your mental health. Plus, it was a COVID floor, and a lot of people died. I would hear them say someone’s coding and sit and worry, ‘Well, am I next?’”
Facing Long COVID-19
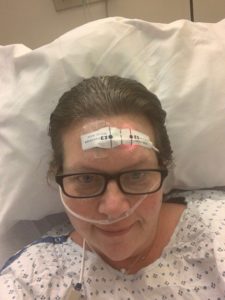 Flynn was strong enough to go home on Christmas Eve.
Flynn was strong enough to go home on Christmas Eve.
“It was a great present,” she says. Unfortunately, she has experienced lingering health problems.
Flynn is now diabetic because of medication that affected her insulin levels, and she lost a lot of hair. She has tachycardia, a condition that causes a rapid heartbeat, and she has difficulty remembering things.
“I have no energy. I used to be able to clean my whole house in an hour and a half, but now I can only clean or mop for about 15 minutes and it feels like I’ve run a race,” Flynn says. “I have to sit down to take a break, breathe and get my heart rate down.”
Flynn has symptoms of post-acute sequelae of SARS-CoV-2 infection, commonly called post-COVID syndrome or long COVID-19, in which patients endure persistent symptoms and health effects of their infection “long after the resolution of the initial infection,” says John M. Baratta, MD, founder and co-director of the UNC COVID Recovery Clinic. Sometimes, these patients are referred to as “long haulers.”
There are no established criteria for what constitutes long COVID-19, other than that a person has to have had a COVID-19 infection and have lingering symptoms that are attributable to it. Doctors typically consider symptoms that last more than four weeks after symptom onset to be lingering, Dr. Baratta says.
The most common symptoms are fatigue, shortness of breath and brain fog, characterized by difficulty with memory and attention. But those certainly aren’t the only possibilities; Dr. Baratta says he treats patients with a wide variety of symptoms across all body parts and organ systems, including headaches, hair loss, tinnitus, chest pain and digestive problems.
Like COVID-19, there are still a lot of unknowns about long COVID-19.
“We don’t really have a clear understanding of the underlying disease process that is causing long COVID,” Dr. Baratta says. “And we don’t have a great understanding of the risk factors. There are some theories about what could contribute to these lingering health issues, but it’s not really understood.”
While long COVID-19 is common in those who have been hospitalized with the virus, it can occur even in people who have had a mild case. Long COVID-19 can last for months or longer—as is the case for Flynn, who also has emotional side effects from her experience.
“I was very outgoing, but COVID takes a toll on your mental health,” Flynn says. “There are certain things that trigger your brain to make you feel those emotions of loneliness and anxiety again.”
Dr. Baratta says the mental health effects of long COVID-19 are common, especially at a time when everyone is under stress.
“When you add having a new, disabling condition related to COVID on top of that, it really compounds the issue, and we are seeing a lot of people who are struggling with anxiety, depression or PTSD after COVID,” he says.
Getting Help
To address her lingering symptoms, Flynn went to the UNC COVID Recovery Clinic, which serves as a central resource for COVID-19 survivors who have ongoing health effects after their initial illness.
The clinic’s thorough intake process determines which symptoms and health effects the patient is experiencing. From there, providers tailor a treatment approach to each person.
“The treatments are really focused on what the patient needs, and that way we can provide some symptom improvement,” Dr. Baratta says.
Flynn goes to cardiac rehab for help with her heart issues and to speech therapy for her cognitive issues. She has since been vaccinated for COVID-19.
Dr. Baratta says that nearly all of the 425 patients evaluated at the COVID Recovery Clinic were unvaccinated when they contracted COVID-19. That tracks with a recent study that found vaccinated people who experience a breakthrough infection were about 50 percent less likely to experience long COVID-19 than unvaccinated people who get infected.
“All of these people in our clinic had not previously been vaccinated when they got COVID,” Dr. Baratta says. “It is so important to get vaccinated.”
Flynn says she encourages people to get vaccinated against COVID-19.
“I promise you, if people knew what it was like to go through this,” Flynn says, “they would get vaccinated.”
If you think you may have long COVID-19, talk to your doctor or contact the UNC COVID Recovery Clinic at (984) 974-9747.