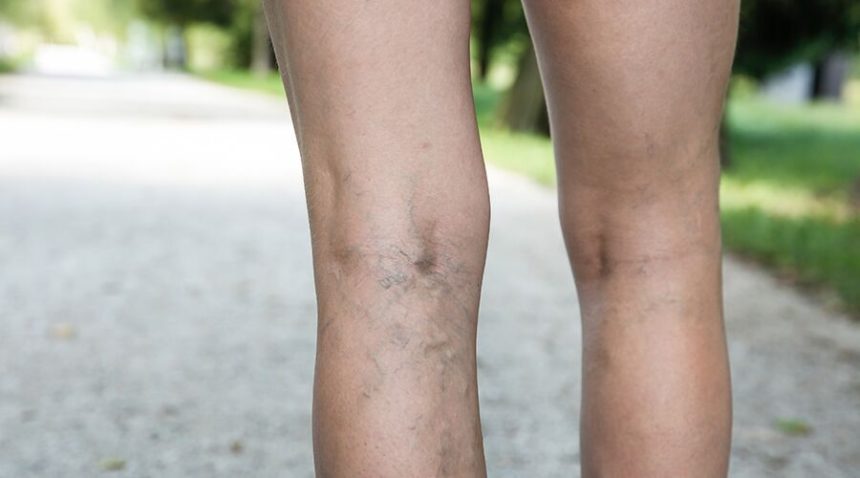
About 20 percent of adults have varicose veins, and most everyone has a spider vein or two. While you may not like the way they look, these bluish, lumpy intrusions are usually harmless. However, for some people, they can be painful and dangerous. We talked to UNC Medical Center vascular specialist William Marston, MD, and UNC REX vascular specialist S. Wayne Smith, MD, to learn more.
Here’s what to know about leg veins.
1. All leg veins are not the same.
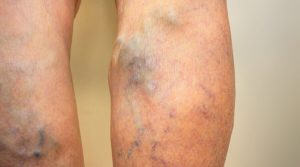
Veins are thin-walled vascular structures with valves that keep blood flowing in one direction: toward the heart. Varicose veins form when valves deteriorate, allowing blood to flow downhill and pool in the leg.
“Veins can lose their elasticity, and when they lose their elasticity, they dilate,” Dr. Smith says. “Veins have valves whose purpose is to keep the blood moving from your foot back to your heart. Valves go bad, the blood goes in reverse and this leads to varicose veins.”
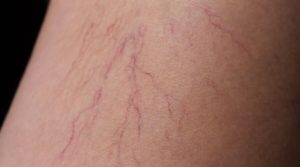
What many people identify as varicose veins are actually spider veins, which are smaller, tubular blood vessels that occur in treelike, spiderweb and starburst patterns.
“These don’t often cause medically important symptoms or put the leg at risk for serious complications, but they don’t look normal and some patients choose to treat them for cosmetic reasons,” Dr. Marston says. “There’s a lot of misinformation on the internet and other places that make people think that they have to treat them, when many times they don’t if they don’t cause pain or other symptoms.”
True varicose veins are bulging, ropy, snaky, abnormal-looking veins that are usually visible to the eye (unless a patient is significantly obese) and often cause painful symptoms, Dr. Smith says. And sometimes they are very serious.
The key to medical management of varicose veins, Dr. Marston adds, is determining which are likely to cause serious health problems requiring intervention and which can be treated conservatively.
2. Some symptoms shouldn’t be ignored.
It is important to seek medical treatment immediately if you experience:
- Hyperpigmentation of the lower leg and ankle, meaning skin patches become darker than the normal surrounding skin
- Thickening and hardening of the skin in the same area that may itch and look red and scaly, similar to eczema
- A skin ulcer, which is a sore that appears red and may drain fluid or pus and is not caused by an injury
“These would be the most severe symptoms where urgent attention is needed,” Dr. Smith says. “Sometimes you develop varicose veins because you had a deep vein clot.”
This is called deep vein thrombosis, and it can cause leg pain or swelling. It also can occur with no symptoms. The most reliable symptom is calf swelling in one leg. Contact your doctor immediately if you have a pain in your leg that starts in your calf and feels like cramping or soreness, if you have red or discolored skin or if your leg feels warm when you touch it. Deep vein thrombosis can be fatal because blood clots can break off and travel to your lungs. Most varicose veins are not related to deep vein thrombosis.
The following symptoms are not urgent or life-threatening, but make an appointment to see a doctor if you experience:
- Achy, heavy legs that are typically relieved when elevated for at least 15 minutes
- Burning, throbbing sensation over an enlarged vein
- Muscle cramping and restless legs at night
- Unexplained swelling in the lower leg and around the ankle
- Any varicose vein that bleeds
Dr. Smith says patients often grow so accustomed to the discomfort caused by their varicose veins that they think symptoms are normal.
“You fix a bad vein, and the patient comes back after the procedure and says, ‘I didn’t know my leg was bothering me until I fixed the vein,’” he says.
3. You’ll probably need an ultrasound.
Dr. Marston says if you have concerns about your veins or painful symptoms, you should go to an expert who specializes in the treatment of vascular problems and get an ultrasound to explore how well your veins are functioning.
“If we identify valve dysfunction that is associated with significant leg symptoms, that generally should be corrected if possible,” Dr. Marston says. “So once we get those tests, we can counsel the patient on the entire picture of what’s causing the vein problems.”
The ultrasound also can help determine whether the vein should be treated surgically, managed medically or left alone, Dr. Marston says. Insurance companies and Medicare usually cover the ultrasound.
4. Many treatment options are available.
Fifteen years ago, varicose vein treatment meant patients had to go under anesthesia in an operating room, but today most procedures are done in the doctor’s office under local anesthesia and with a light sedative, Dr. Smith says. Treatment usually lasts one hour, and you are active the next day.
Three treatment options are available for large varicose veins, what Dr. Smith calls “the ropy veins.”
The first treatment, called radiofrequency ablation or laser ablation, involves using a catheter to numb the leg and then heat the vein until it’s closed. Local anesthesia is used around the vein to prevent nerve damage and burning the skin.
“This can be done with no surgical incisions, just a small catheter to gain access into the vein, and that allows us to close it,” Dr. Marston says.
Another treatment option is to glue the vein.
“We still use a catheter, but we put a glue inside the vein that glues the vein shut,” Dr. Smith says. For this procedure, you don’t have to anesthetize the leg and there’s no risk of nerve damage from heat.
A third treatment option, sclerotherapy, uses a chemical foam to close the vein. Using ultrasound, the physician finds the vein and places an IV into it.
“Then we move the bed to position the patient’s head down with the legs raised. Their legs are positioned about 8 inches above their heart so the vein can be massaged free of blood,” Dr. Smith says. “Then we inject the chemical foam, and when that hits the wall of the vein, it collapses it.”
The type of treatment selected depends on the patient’s anatomy.
While these treatments are medically necessary because the affected veins usually have an underlying valve problem, there are other options for veins that are treated for cosmetic reasons.
“If it’s all in the little spidery bluish things you see, which are called superficial veins, then typically those problems can be treated with laser or other methods to close the vein that has the abnormal valve in it,” Dr. Marston says.
Using a vein light to illuminate the skin, the physician finds the vein and uses a tiny needle to inject foam into it. This makes the vein collapse. The collapsed vein is reabsorbed into surrounding tissue and eventually fades.
Another treatment option, Cutera, uses a laser to destroy the vein.
“We use that when the veins are so small that you can’t get into them with a needle,” Dr. Smith says.
All these procedures require wearing compression hose for about a week afterward. While veins treated for medical reasons are generally covered by insurance, veins removed for cosmetic reasons are not.
5. Veins may be inevitable, but diet and exercise can help.
Spider and varicose veins are common, Dr. Marston says.
“Particularly as we age, most of us will have some veins that are visible or look abnormal,” Dr. Marston says.
Experts don’t know exactly what causes varicose veins, but there are known risk factors, including obesity, genetics and working a job that requires continuous standing.
“There’s a very strong genetic predisposition to varicose veins,” Dr. Smith says. “So if your mother at age 50 had to have her veins fixed and you are worried about what’s going to happen to you, preventive measures are weight control, exercise—even just trying to walk 30 minutes a day—and try to avoid standing or sitting particularly in one position for long times. Also, wear a low-compression support hose (20-30 millimeters).”
6. Veins that spring up during pregnancy may go away on their own.
Varicose veins often are triggered by pregnancy.
“Circulating blood volume goes up to take care of the baby, and the hormonal changes cause dilatation or stretching of veins,” Dr. Smith says.
Wait three to six months after you deliver your baby to seek treatment for pregnancy-related veins, Dr. Smith says, because they often regress and will not need treatment.
If you are concerned about varicose veins, talk to your doctor. UNC Health Care has vein treatment options in Orange and Wake counties.