If you’ve put off receiving a recommended cancer screening, it’s time to get it scheduled. These screening tests can detect cancer in its earliest stages, when it’s easier to treat and leads to better outcomes.
“The old adage ‘an ounce of prevention is worth a pound of cure’ really applies here,” says UNC Rex breast cancer specialist Oludamilola “Lola” Olajide, MD. “If we can screen to make sure that we detect such cancers early, it will often ensure that the patient has less trauma from extensive therapy, and it will also most importantly ensure that the individual has a better chance at surviving the cancer. Early detection is really very important.”
Here’s what you need to know about essential cancer screenings.
Early Detection of Breast Cancer Begins with an Annual Mammogram
One in 8 women in the United States will develop breast cancer. It’s diagnosed more than any other type of cancer and is the second-leading cause of cancer-related deaths for women in the United States. Black women have a higher rate of death from breast cancer than white women.
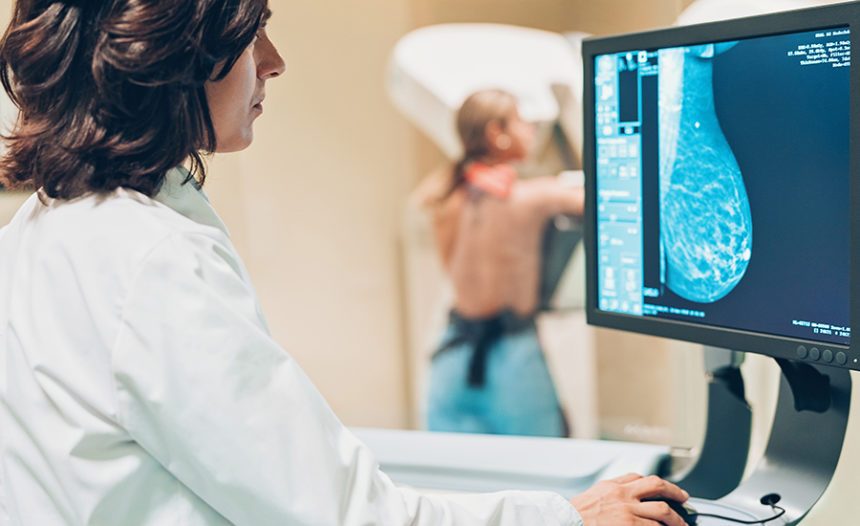
A mammogram is the best weapon for catching breast cancer at an earlier, more treatable stage.
“The goal of doing a yearly screening mammogram is that we’re hoping to pick up pre-cancerous and cancerous changes before they become a mass you can feel,” Dr. Olajide says. “And if a cancer is found, we’re catching it in the earliest stages, when it requires less aggressive treatment.”
Women should mammograms starting at age 40 and continue every other year through age 74.
For women at higher risk of breast cancer—for example, because of family history—mammograms should begin earlier, possibly in the late 30s. Talk to your doctor about when you should begin your screening mammogram.
Bottom line: Schedule your annual mammogram. If you don’t yet get mammograms, talk to your doctor about your risk and when you should start.
Colonoscopies Prevent and Detect Colon Cancer
Colon cancer is the third-leading cause of cancer-related death in the United States, but it’s also one of the most preventable cancers, thanks to a screening tool called a colonoscopy.
A colonoscopy not only detects colon cancer, it can prevent it, too. During a colonoscopy, doctors look for precancerous or cancerous colon polyps in the lining of the colon. If doctors spot these growths, they can quickly and painlessly remove them during the colonoscopy.
New guidelines call for colorectal cancer screening starting at age 45 if you’re at average risk.
If you have a family history of colon cancer, colon polyps or high-risk disorders that predispose you to colon cancer, you should be screened at a younger age, typically at age 40. This includes people with inflammatory bowel disease, including ulcerative colitis and Crohn’s disease.
Colorectal cancer disproportionately affects the Black community, whose rates are the highest of any racial or ethnic group in the United States. African Americans are about 20 percent more likely to get colorectal cancer and about 40 percent more likely to die from it than most other groups. For that reason, African Americans should be screened at age 45 or sooner, depending on family history.
Bottom line: Talk to your doctor about your risk. If you are due for a colonoscopy, get it.
Pap Tests Can Detect Precancerous Cells in the Cervix
Cervical cancer was once one of the most common causes of cancer death for women in the United States. The cervical cancer death rate dropped significantly with the increased use of the Pap test, which can detect changes in the cells of the cervix before cancer develops or when it’s small and easier to cure.
In the United States, cervical cancer is one of the most preventable cancers. There are two screening tests for cervical cancer: the Pap test and the HPV test.
The American Society for Colposcopy and Cervical Pathology recommends that women have a Pap test every three years beginning at age 21. After age 30, HPV testing is preferred. The frequency of cervical cancer screening depends on your likelihood of having cervical precancer or cancer and is based on your medical history.
Researchers have found that the HPV test may detect abnormal cervical lesions earlier and more accurately than the Pap test alone. For women age 30 and older, a Pap test alone is acceptable only if HPV testing is not available. In those circumstances, it should be performed annually.
Bottom line: Talk to your doctor about whether you are due for a Pap test or an HPV test.
Call Your Doctor if You Have Any Cancer Symptoms
If you have a concern such as a lump in your breast, blood in your stool or abnormal vaginal bleeding, call your doctor immediately. Don’t delay treatment without first consulting your doctor.
“People often have a fear around screening because they are concerned that if they get tested, we may find something. But if you do in fact have a cancer, having found it early often will ensure a better outcome from that disease,” Dr. Olajide says. “So it is really important not to bury our heads in the sand, and if you are eligible for a certain screening procedure, get it done at the appropriate time.”
If you’re concerned about your cancer risk, talk to your doctor. If you do not have a doctor, find one near you.