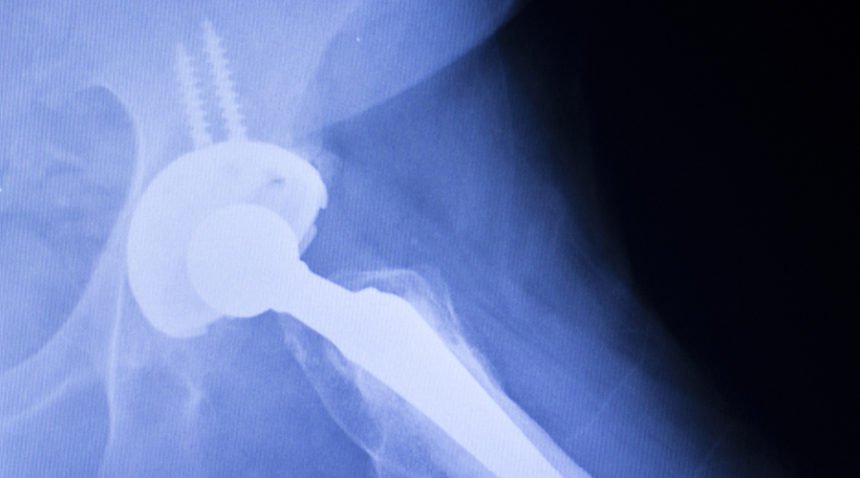
If you’ve had a knee, hip or another joint replaced, you’re in good company. Total joint replacement, in which an arthritic or damaged joint is replaced with a prosthesis, is one of the most common surgical procedures performed in the United States. What was once considered a surgery only for the old is now regularly performed well before a person’s 65th birthday.
About 800,000 knee replacements and more than 450,000 hip replacements are performed in the U.S. each year. With such high numbers and patients living longer, it’s not uncommon for people to require a revision joint replacement surgery.
Joint replacements sometimes last decades, but in about 4 or 5 percent of patients, the original prosthesis will need to be replaced within 10 years. Other people will need such a surgery after 15 or 20 years. This can be because the implant has worn out, or because of infection, scar tissue or a fracture.
To find out more about joint replacement revision surgery, we spoke with Christopher W. Olcott, MD, a UNC Health orthopedic surgeon who specializes in joint replacement. Here he helps to answer some of the most frequently asked questions.
How long do joint replacements usually last?
“Most joint replacements last anywhere from 15 to 25 years, but that is very dependent upon how active the patient is,” Dr. Olcott says. “Joint replacements don’t last as long in people who are highly active.”
A study published in The Lancet in 2019 found that about 82 percent of total knee replacements last 25 years. A similar study found that a hip replacements will last 25 years in about 58 percent of patients.
How do you know if your joint has failed?
“Patients in the early stages of joint replacement failure are asymptomatic but develop pain with activity in the later stages,” Dr. Olcott says.
Some of the warning signs of joint replacement failure include:
- Pain that comes on suddenly in the affected joint
- Decreased range of motion
- Stiffness
- Swelling
- Trouble getting around because the joint replacement is no longer working as well as it did before
If you experience any of these problems, see your orthopedic surgeon as soon as possible to get it checked out, Dr. Olcott says.
What is involved in a revision surgery?
In a revision surgery, the doctor removes some or all of the parts of the original joint replacement and puts in new parts. It is a longer and more complicated procedure than the first, or primary, joint replacement.
“Revision surgery is a complex procedure requiring prolonged operative time with special implants,” Dr. Olcott says. “There is also an increased risk of infection, and the results of revision surgery are often not as good as with the primary procedure.”
What is recovery for a joint revision surgery like?
“There is a prolonged recovery period after a revision surgery. It usually takes at least double the time to recover compared to a primary procedure,” Dr. Olcott says.
Your mobility will be limited for several weeks after revision surgery. During this time, you will need help from others with daily activities such as cooking, bathing and shopping, so plan for this in advance. Your healthcare team may be able to help you make arrangements for someone to assist you at home.
Depending on the severity of your case and your condition after revision surgery, you may need to spend some of your recovery time at a nursing facility or rehabilitation center after you leave the hospital.
How should people getting joint replacements plan for future surgeries?
“Ideally, most people should delay joint replacement surgery until they reach the age of 65 to 70,” Dr. Olcott says, to reduce the possibility of needing a revision. “But many patients are unable to wait this long.”
With people getting replacements at younger ages, it becomes more likely they’ll need a revision surgery.
“It’s best to try to take care of your total hip or knee replacement, but often revision surgery is unavoidable,” Dr. Olcott says.
To extend the life of your implant, avoid high-impact exercise that pounds your joints, such as running, Dr. Olcott says. Instead, try walking, bicycling, using an elliptical machine and resistance training. If you’re overweight, it will help to lose weight, Dr. Olcott says. It’s also important to try to avoid skin infections near the joint replacement; keep any wounds clean, and seek medical attention immediately if you suspect infection.
Talk to your doctor about any joint pain or mobility problems you experience. Need a doctor? Find one near you.