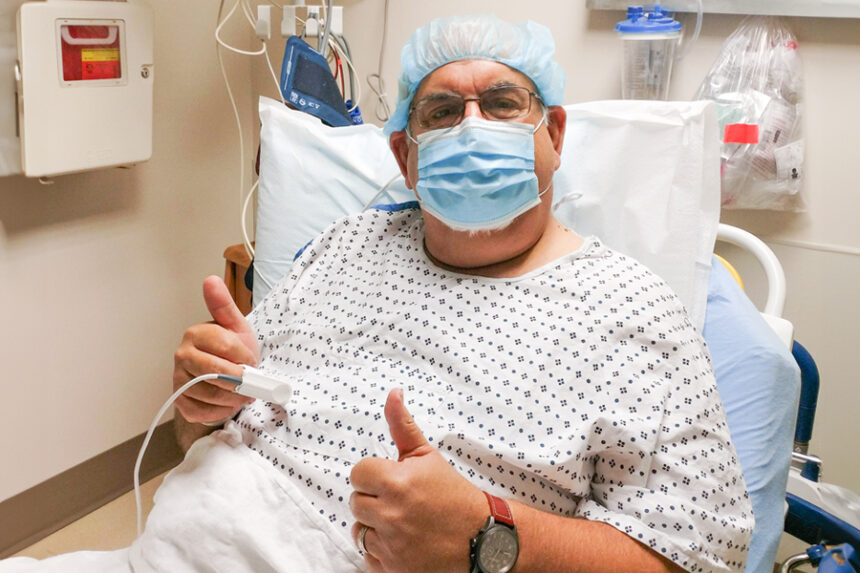
In fall 2020, John Bell noticed some swelling on the side of his neck, and when he had trouble swallowing, he knew it was time to see a physician. An otolaryngologist—also called an ear, nose and throat doctor, or ENT—said he thought Bell had a squamous cell carcinoma, a type of skin cancer.
“My whole life passed before my eyes,” Bell says. “You hear people say that, but it really happened to me.”
A few days later, a scan and biopsy revealed Bell’s diagnosis as diffuse large B-cell lymphoma, an aggressive cancer of the lymphatic system, and he began six months of chemotherapy. Although Bell says he felt good during treatment, the chemotherapy had no effect on the cancer.
“You never want to hear an oncologist say that a scan doesn’t look great,” Bell says. “I had never considered the possibility that chemo wouldn’t be successful, so I was devasted when it didn’t work.”
Pursuing CAR T-Cell Therapy
Bell was referred to Natalie S. Grover, MD, clinical director of the Cellular Therapy Program at UNC Health, in summer 2021. Because Bell’s lymphoma was resistant to chemotherapy, he was a candidate for a type of immunotherapy known as chimeric antigen receptor (CAR) T-cell therapy. A person’s blood is drawn, and the T-cells—white blood cells—are manipulated in a laboratory to include a protein that helps the cells find and destroy cancerous cells. The engineered cells are then infused into the person.
“I worked in a medical lab for 37 years, so I’m not a stranger to this type of thing, but I was worried about infection and long-term side effects,” Bell says.
Side effects of CAR T-cell therapy include cytokine release syndrome, which can cause fever, low blood pressure and low oxygen, and immune cell-associated neurotoxicity, which can cause confusion and speech problems and sometimes seizures, brain swelling and coma.
“We require that a caregiver be with our patients after their transfusion so they can be monitored for these side effects,” Dr. Grover says. “It’s something we watch very closely.”
After weighing the risks, Bell decided to pursue the therapy. Before his infusion, he underwent two rounds of chemotherapy: a bridging therapy to keep his disease controlled and a conditioning therapy to prepare his body for the CAR T-cells.
When Bell received his CAR T-cells in November 2021, he initially felt fine. A few days later, however, he was admitted to the intensive care unit with neurotoxicity.
“They told me not to panic. I have no recollection of the three days I spent in the ICU, and that’s probably for the best,” he says.
“Neurotoxicity can be the most distressing part for patients and their families,” Dr. Grover says. “We provide counseling ahead of time, but it’s still hard to deal with. Patients usually don’t remember it, and the burden is on the family members while we manage it.”
She says that different CAR T-cell products have different risks for neurotoxicity, and research is being done on treatments to help prevent and reduce the severity of neurotoxicity.
Remission Through CAR T-Cell Therapy
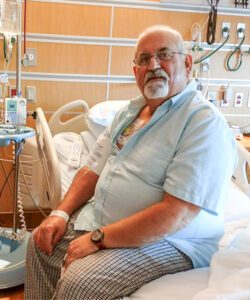 Just a month after receiving CAR T-cell therapy, Bell’s scans revealed he was in complete remission.
Just a month after receiving CAR T-cell therapy, Bell’s scans revealed he was in complete remission.
“My life has returned to how it was pre-cancer,” he says.
The 69-year-old enjoys relaxing, cooking and spending time with his family. Retired from full-time work, he works part time.
“This treatment provides hope for patients who did not respond to initial treatment or who have had a relapse,” Dr. Grover says, noting that excellent outcomes such as Bell’s aren’t guaranteed. About half of people respond to CAR T-cell therapy. Researchers are working to identify the factors that predict a good response.
Advice for People Considering CAR T-Cell Therapy
Bell advises people considering CAR T-cell therapy to find a medical team that they trust.
“You’re your own best caregiver, so don’t be afraid to ask a lot of questions,” he says.
He also found comfort in an online CAR T-cell support group, which he says “was a huge help to me.”
Bell knows his other piece of advice is easier said than done: He wishes he had worried less.
“I realized that a lot of my fear about the treatment was in the not knowing,” he says. “Other than those three days in the ICU, the process was a breeze, but I spent a lot of time worrying about what might happen. We should try not to worry about something until it actually happens.”
If you have questions about cancer treatments, talk to your doctor. Need a doctor? Find one near you.