With only one physician in Malawi trained to perform the surgical procedure required to treat cervical cancer—radical hysterectomy—women died in large numbers from the disease. Two UNC OB-GYNs came up with a way to change that.
Dr. Lameck Chinula knew completing 10 major surgeries in five days was ambitious, but that was all the time he had.
Two U.S.-trained gynecologic oncologists had arranged to travel to Lilongwe, Malawi—the nation where Dr. Chinula practices medicine and calls home—for just one week to teach him the hands-on surgical skills he’d need to address one of his country’s most pressing problems.
Malawi and sub-Saharan Africa are “the epicenter of preventable cancer death,” said Dr. Chinula. A lack of screening services, late presentation to health facilities, high burden of infectious diseases, complex pregnancies and lack of human resources all play a role. With only one physician in Malawi trained to perform the surgical procedure required to treat cervical cancer—radical hysterectomy—women died in large numbers from the disease.
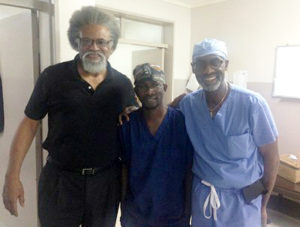
A radical hysterectomy can take four or more hours for even an experienced gynecologic oncologist working in a highly resourced facility. With Dr. Chinula just learning, he might need five or six hours per case, times 10. It was overwhelming, but he wanted to do for the women of his country what these doctors—UNC OB-GYN’s Zambia-based gynecologic oncologist Dr. Groesbeck Parham and Dr. Michael Hicks, a gynecologic oncologist from Michigan—could do. He wanted the skills that would enable him to stand between his patients and needless death.
“I remember by Wednesday of that week feeling like I’d been doing some kind of intensive gym training for a Mayweather-type boxing match,” said Dr. Chinula, the first Malawian OB-GYN at UNC Project Malawi. That Friday in June, he would perform the 10th surgery alone to become the only physician in Lilongwe, and only the second in Malawi, who could provide the surgery proven to cure early-stage cervical cancer.
Dr. Chinula says he can still see the smiles of the doctors, the nurses, and of all those who had come to the operating theater to observe the final surgery. Dr. Hicks joined him at the table just before he closed the abdomen to check his work. Dr. Chinula had made it through the week, and 10 women had been offered a surgery that, thought routine in western nations, had been unavailable in theirs.
Dr. Chinula was exhausted, but proud—he had fought and won another fight for the women of his country.
“You cannot imagine the number of lives we will now be able to save,” he said.
Empowering women through healthcare
For Dr. Chinula, saving lives in the land he loves is borne from a desire to influence women’s experiences in Africa, to uplift and support them.
“When I was growing up, I realized how much difference a mother makes in the lives of her children,” he said. “I realized that if I could ensure that women are healthy and empowered through education, they have a better chance of making the world a better place for everyone.”
He wasn’t sure, at first, how he’d do that. Then, he decided he could become a doctor, with a focus on women’s health. After that, it was something more. To make a lasting difference in the lives of African women, he needed a career where he could engage in research, literature and evidence-based practices.
“This is where UNC Project Malawi comes in,” Dr. Chinula said.
UNC Project-Malawi is a collaboration between UNC-Chapel Hill, the Malawi Ministry of Health, and the Malawi College of Medicine. The project is based on the campus of Kamuzu Central Hospital in Lilongwe. Through educational partnerships UNC Project-Malawi has with the National Institutes of Health (NIH) Fogarty AIDS International Training and Research Program and the Gilead Training Fellowship, Dr. Chinula completed his OB-GYN residency training at the University of Cape Town in South Africa.
Upon Dr. Chinula’s return to Malawi in November 2014, he met Dr. Parham for the first time, at a meeting in Lusaka, Zambia. That meeting would set things in motion.
Dr. Parham has been living and working in Zambia as a gynecologic oncologist for the past 11 years, and in Africa since 1985. On faculty at UNC OB-GYN and a member of UNC’s Lineberger Comprehensive Cancer Center, he received a National Cancer Institute (NCI) grant last year aimed at building a cancer-related research platform between the UNC sites in Zambia and Malawi. Dr. Chinula went with two other doctors to Lusaka to meet with Dr. Parham.
“I informed the team about our lack of treatment options for cervical cancer. There is no radiotherapy, and chemotherapy is limited. Our hospital had no one trained to offer radical hysterectomy for early stage cervical cancer,” said Dr. Chinula.
The two doctors realized that, with funding and a willingness to make it work, Dr. Parham could pass his skills to Dr. Chinula and extend the reach of care from Zambia into another African nation.
“Cervical cancer is the number-one cause of cancer-related death throughout sub-Saharan Africa, and because of these circumstances, the vast majority of Malawian women diagnosed with cervical cancer die without any form of treatment,” said Dr. Parham. “The numbers of formally trained gynecologic oncologists in Africa can be counted on one hand—I’m the only one in Zambia—and the opportunities for Africans to acquire such training in the western hemisphere are virtually nil.”
And, Dr. Parham predicted, the situation would soon worsen. Malawi had recently established a cervical-cancer screening program, which meant more women would be diagnosed, though unable to access treatment. He engaged a lifelong friend, colleague and former student, Dr. Hicks, a gynecologic oncologist from Michigan who visits Africa to work with Dr. Parham several times a year. The two traveled to Lilongwe to train Dr. Chinula.
“As a result of the training, the capacity to surgically treat women with cervical cancer in Malawi immediately increased by 100 percent.”
“As a result of the training, the capacity to surgically treat women with cervical cancer in Malawi immediately increased by 100 percent,” said Dr. Parham.
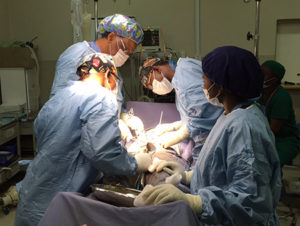
In one of the world’s poorest and most resource-constrained countries, patient after patient was able to undergo a surgical procedure which was potentially life-changing, and which could not have been performed in the past.
Dr. Parham said with each completed procedure, the pride in the operating room grew.
“Each day as the understanding and awareness of what was actually happening—two master pelvic cancer surgeons from the U.S. were infusing their surgical knowledge and skills into the hands and brains of a Malawian doctor—the camaraderie grew,” he said. “In the process, we transcended our circumstances.”
An impact, amplified
As a result of the training, huge gains in women’s health were made in Lilongwe, Malawi, and Drs. Parham and Hicks gained not only a trainee and a sense of pride in what they’d been able to do for the region, but also a partner and colleague. Dr. Chinula joined the UNC OB-GYN faculty as research assistant professor on July 1.
“He brings brilliance, a new form of energy, a desire to know and to make research contextually relevant to patient care,” said Dr. Parham. “He represents a conduit for us, his mentors, to pour what we’ve been privileged to learn into a part of the world where people have been overlooked, largely forgotten or written off as insignificant.”
The appointment allows Dr. Chinula to further his research mission and to continue to work with experienced UNC faculty in his search for more evidence-based interventions to benefit Malawian women. The colleagues plan to work together as often as time and funding allows, and collaborated as recently as September on another cancer that is increasing among young HIV-infected women—cancer of the vulva.
Dr. Parham wants to train even more doctors in Africa and is currently raising money for a surgical training center based in Zambia that will train many OB-GYN physicians, like Dr. Chinula, from the surrounding region. There’s more to do—though they will need more time and more money. Dr. Parham believes, though, it will come.
“In situations of severe human suffering and broken medical systems where something is always missing or malfunctioning, and there is never enough of anything, it’s easy to give up. What these doctors are asked to do, and the conditions in which they are forced to work are unfathomable,” he said. “For those of us who have the opportunity and privilege to work side-by-side with our African colleagues, it is our responsibility to represent hope and the possibility of excellence.”
